DEVELOPING NATIONAL OBESITY PREVENTION POLICIES: AN INTERNATIONAL PERSPECTIVE
France has clearly developed a great number of initiatives since the time of the last French Presidency of Europe when it attempted to support a new strategy for nutritional policies in Europe by convening the Eurodiet project with the EU Commission (Eurodiet, 2001). The senior French diplomats were initially in agreement with the concept of a collaborative effort being undertaken between a group of top nutritionists from different EU countries and the major representatives of the European food industries. The plan was to evaluate what was nutritionally best for public health and the future of all the populations of Europe whether living in the far North or in the Mediterranean area. Much was being made of the value of the Mediterranean diet and the fact that the Greeks, Italians and French in particular had a better health record than those populations living in other countries.
Developing public health analyses and policies: the importance of being independent of industrial interests
Unfortunately it soon emerged that the development of a coherent approach to specifying an optimum European diet in the Eurodiet project was becoming difficult to establish because of repeated objections from a couple of scientists who had been proposed as suitable contributors to the development of the public health analyses by the food industry. The rest of the group were well aware of the regular funding of these scientists by the food industry - and particularly by the soft drink, confectionary and sugar interests - but their numerous objections and alternative suggestions still had to be dealt with on the basis of reasoned, detailed and often extensive arguments.
The majority of the nutritional scientists and public health specialists were very clear that great efforts were needed to limit the amount of fat, particularly saturated fats, sugars and salt being consumed by Europeans, an analysis in agreement with all other major governmental and World Health Organisation (WHO) reports (WHO, 1990, 2003). Once most of the analyses had been agreed a special conference was convened in Crete so that in an open public discussion the public health implications of the reports could be evaluated. Again, however, the French diplomats were dismayed to discover the intensity of the objections to the agreed analyses by industrial groups and how the conference was being misled about supposed official meetings of the Chief Dental Officers of Europe who seemingly had proposed a more benevolent approach to current national sugar intakes. In practice a meeting of some dental officers had occurred but this was a meeting funded by sugar interests and without any official status. Even more disturbing was the continued resistance of official EU representatives from the Commission's Directorate involved with trade to the then agreed official WHO policy on the value of a minimum of 6 months breast feeding. From this experience and the subsequent intense lobbying of the Commission to set aside the Eurodiet conclusions most governments and the Commission have now come to recognise that public health and nutritional analyses together with their policy implications need to be developed completely independently of industrial interests.
This conclusion has been reinforced by the experience of the Bovine Spongiform Encephalopathy (BSE) crisis with which I was completely involved as a scientific expert first for the UK Prime Minister, Tony Blair (James and McColl, 1997) and then for the Commission. The BSE crisis at that stage was so serious that it led to the threat to sack the European President and his Commissioners. The Commission responded with a total reorganisation of the Commission's approach to health and the development of DG SANCO with a clear mandate to put the interests of the population's health above the immediate concerns of trade and other powerful lobbies. In the case of BSE we in the Commission's Scientific Steering Committee were constantly under pressure with Chief Veterinary Officers complaining about our conclusions and sometimes seeking our expulsion from our job as we identified one after another EU country as probably having BSE and not taking adequate precautions. The Commission at that stage insisted on the value of our independent analyses and soon realised that their best insurance against charges of neglect was to automatically back our opinions. This approach was rapidly reinforced when we were repeatedly shown to be correct in our meticulously prepared analyses which contradicted most if not all the claims and counterarguments of farming groups and those involved in the distribution and processing of meat products.
This experience of BSE has led the EU Commission in DG SANCO to recognise that scientific analyses and options for policy development in relation to health or other consumer or general public interest need to be developed by a thoroughly independent group of experts. This does not mean, however, being anti-industrial - a common charge when the conclusions do not favour particular interest groups. Indeed industry has a major role to play in being involved in the policy implementation process and in highlighting particular options which would allow the least adjustment to their current practices but still meet the objectives of a new policy. Thus on March 15 th 2005 the Commission announced the formation of a joint Commission/industrial/non-governmental organisation (NGO) Platform for the prevention of the current alarming rates of obesity in Europe. All sectors of the European food industry are involved but the Commission is very clear that any nutritional policy needs to be developed by an independent group and not by those with a special financial interest. In keeping with this policy the decision of the French Parliament to commission an independent report from Inserm on possible new analyses of nutritional public health needs in France is to be welcomed.
Nutritional needs for combating obesity and their policy implications
It is only since 1997 that WHO and then many national governments have come to recognise that obesity is now a major public health problem affecting not only North America and Europe, but most of the developing world (WHO, 2000). The European Regional Office of WHO has also now established obesity as its top priority and this issue will be considered by all the Ministers of Health for the WHO European Region in Istanbul in November 2006. It is therefore clear that there has been very little time so far for major initiatives to be undertaken to combat obesity and policy makers should therefore not be surprised by the very limited information that we have on practical community developments which are known to be successful. Governments throughout the world are now exploring what best to do and it should be recognised that developing public health policies to combat obesity is a much more complex process than we originally expected. In the health field policy-makers have come to demand rigorous multiple double-blind trials of any intervention strategy, e.g. for changes in the use of drugs, when introducing new diagnostic tools or other initiatives. However, when we are dealing with the implications of obesity one has to take a much broader perspective. This broader perspective is dependent on recognising that community intervention projects are much more difficult to conduct than simple drug trials. They also involve many different factors and non-medical sectors which are not readily evaluated in a rigorous, experimental way. Therefore, as with most other aspects of Government policymaking e.g. for social and economic policy making, one has to work on the basis of understanding the causes of the problem, evaluate the primary drivers and then identify suitable options for changing the environment.
Individual or community approaches?
Too often governments and policy makers have considered obesity to be the responsibility of individuals. Surely, they argue, if somebody puts on weight, then they should themselves be able to identify this problem and to prevent any further weight gain and, indeed, return to their previous normal weight by simply eating less and exercising more. Whilst this is biological logical, it neglects the now overwhelming evidence that to assign the responsibility only to the individual is to neglect the huge pressures on the whole of society to put on weight. It is very clear from numerous studies over the last 3-4 decades that obese individuals have been trying desperately to reduce their weight unsuccessfully despite many major educational campaigns, numerous targeting articles in women's magazines and with the popular press focussing on the problem. Despite these efforts and the development of a multi-billion Euro slimming industry the proportion of individuals becoming overweight and obese has gone up inexorably.
Clearly, there are family associations in the propensity of individuals to gain weight. Thus the chances of child becoming overweight are far greater if the child's parents are obese. Whereas traditionally we assumed that this simply reflected bad parenting and the consumption of an inappropriate diet with too little exercise, it has now become clear that families on a similar diet and exercise pattern show very different propensities to weight gain and the genetic susceptibility of different individuals is now well accepted. Thus 20 years ago in France only the very genetically sensitive individuals tended to become obese, but now far more less susceptible people are also becoming obese. It is clear that the genetics of the French population has not materially changed in the last 50 years, so the overwhelming epidemic of obesity has to be of environmental origin. Therefore, to tackle the underlying causes of the epidemic, an environmental approach to prevention is needed and those who gain weight easily need to be in a better environment if they are going to cope effectively with their weight problem.
Why then do obese individuals find it so difficult to return to their normal weight? Under normal circumstances the brain regulates food intake extremely well and we subconsciously adjusts our intake on a daily basis to take account of the variations in the level of physical activity. Thus when somebody puts on weight, this means that the pressures to gain weight have overwhelmed the appetite control system but with a steady 1 kg weight gain each year this still amounts on average to an excess intake of 20 kcals per day, i.e. only 1 % of the usual 2,000 kcal daily intake. This small discrepancy highlights just how effective our normal appetite control system is unless we overwhelm it by taking foods which trigger a poorer response in the complex brain control system and this mechanism has to work even more effectively if we are inactive and therefore demanding that the brain mechanism should stop us eating. Thus when people put on weight it is not because they are foolish or unable to control their food intake - all of us have a sensitive and effective system but a system which we overwhelm by living in an inappropriate environment where there are constant inducements to eat and do very little physical work.
Once we begin to gain weight the brain in some unknown way adapts to the weight gain and then "resets" the normal brain control mechanisms so that the normal control of food intake is geared to maintaining the excess weight. This is why very obese individuals who successfully lose weight only manage to keep their weight at a normal level by obsessively monitoring their intake and deliberately undertaking far more exercise than normal. A constant theme of these "post-obese" individuals is their constant hunger and desire to eat; they then have to go to very special lengths to stop themselves eating when there are so many temptations provided everywhere to eat and drink more than they need. They are also handicapped by their environment where we have all become used to using motor cars, computers, mechanism aids at work and at home. In fact, it is very unusual for anybody now to have to engage in heavy physical work: most of us can earn a very good living without having to be physically active at all.
Thus individuals who are genetically sensitive to obesity are now in particular difficulty because their whole environment is geared to promoting weight gain. This dilemma highlights the fundamental importance of taking a prevention approach to obesity and indicates that in obesity-prone families they will need to systematically develop their own micro-environment to resist the pressures to eat too much and to exercise too little.
The burden and health costs of obesity
In a recent analysis for WHO we assessed the health impact of excess weight gain in different parts of the world (James et al., 2004). Figure 1 shows the burden in different parts of Europe, this burden being calculated in terms of the number of Disability Adjusted Life Years (DALYs) lost and the reasons why overweight people either die early or become sick and disabled. Although there are over 50 complications of excess weight gain and obesity, we only had very clear data on the greater rates of ischaemic heart disease (IHD) high blood pressure (HT), stroke, diabetes and 3 forms of cancer, i.e. colon, post-menopausal breast and endometrial cancer. We were able to add the problem of arthritis induced by weight gain, but could not take account of all the other disabilities that relate to excess weight e.g. backache, respiratory impairment and numerous other conditions. Figure 1 shows that in the Euro A region, which includes France, there are nearly 2 million lives lost or disabled each year in both men and women due mainly to the cardiovascular disease and diabetes induced by excess weight gain. In these calculations no separate national analyses were made, but it is clear that these estimates need to be looked at both in terms of the recognised huge increase in the health burden that is likely to occur in France and elsewhere over the next 20 years and, indeed, the economic costs of the health burden. So far we have failed to recognise the health costs of obesity which the UK National Audit Office (National Audit Office, 2001), the British Parliamentary Health Select Committee (House of commons health Committee, 2004) and, indeed, the UK government's own special economic advisor, Derek Wanless, has recently highlighted (Wanless, 2004). Indeed these costs are probably major underestimates because it is now becoming evident that we have failed to take account of just how much the escalating epidemic of diabetes will impact on the problem of kidney failure: there is going to be a huge increase in the demand for kidney dialysis. The cost of dialysis is estimated at 40-50 thousand Euros per year for the dialysis part of the medical care alone and already up to a half of all patients in dialysis units have diabetes as the underlying cause. Type 2 diabetes is now so closely linked to excess weight gain and obesity that the term "diabesity" has been coined to emphasise the intrinsic linkage. Our own analyses of the time when the burden from overweight and obesity is at its greatest shows that it is in the 45-59 year old group where the maximum disability is evident, i.e. during the economic working life of the population. Indeed, over 70% of the total burden is seen in those below the age of 70, so this is not a problem of the very old: it is a problem which is already affecting the working capacity of the population. The UK government has very recently assessed the impact of obesity as already leading to an average reduction in the UK population's life expectancy of 2 years (Department of health, 2004).
Euro A: EU, Croatia, Czech, Norway, Switzerland
Euro B: Bulgaria, Poland, Romania, Turkey, Balkans, some Asian republics
Euro C: Baltic countries, Hungary, Russia, Ukraine, Belarus, Kazakhstan, Moldavia
.
DALYs
X 10
3
Euro A
Euro B
Euro C
Euro A
Euro B
Euro C
Sub
-
region
0
500
1000
1500
2000
2500
3000
MEN
WOMEN
Arthritis
Endomet
.
Ca
.
Breast
Ca
.
Colon
Ca
.
Diabetes
Stroke
HT
IHD
Figure 1 : Disease burdens in Europe linked to increasing body weights
The DALYs are calculated on the basis of the years of life lost And the years of disability induced every year in that proportion of the population which is above the optimum average corresponding to a BMI of 21.0. The proportion of the specified diseases attributable to this excess weight gain is then derived from independent studies and in these calculations have been limited to the impact of weight gain on the development of ischaemic heart disease (IHD) high blood pressure (HT), stroke, diabetes mellitus, cancers of the colon, endometrium (uterus) and breast in post-menopausal women together with the impact on arthritis.
Developing a physical activity prevention strategy: the need to redesign our towns and cities to allow routine walking and cycling as part of every-day activity
Developing a strategy depends on a clear analysis of the underlying causes of the obesity epidemic. First, consider the problem of physical activity where it is now clear that the old idea that we should engage in perhaps 30 mins of moderately vigorous activity e.g. fast walking, 5 times a week does indeed help to reduce the risk of cardiovascular disease but to prevent weight gain, particularly after some weight loss, then 60-90 minutes extra walking is needed for the majority of the population (Food and Agricultural Organisation of the United nations, 2001). Now the pressures to remain without physical activity are many including all the easy transport systems, the work environment and the inducements to stay at home, watching television or working with games and other internet systems.
Given these huge environmental changes no one would suggest that these developments be reversed but we need to recognise the billions of Euros of public and private investment in the reorganisation of the transport systems of all developed countries with a road and urban redesign which has been primarily to ease and speed the flow of motor cars. So how should we respond? There has already been an attempt to encourage people to exercise more, to engage in sports and other recreational activities. In response to this campaign it is clear that sub-groups within the better educated and wealthier sector in our societies do develop a new leisure time approach to physical activity. Special leisure centres have been constructed with appreciable numbers paying extra for the privilege of access. However, almost everywhere it is clear that the numbers actually engaging in routine physical activity are small and on a population basis there is no evidence of a systematic increase in physical activity patterns. Furthermore the emphasis on an educational approach to taking extra physical activity during leisure time impacts only on a minority; the main beneficiaries are those in the higher social class who have the ability and resources to alter their lives despite all the current constraints on routine physical activity in our daily life. Thus the routine demand to tackle the problem of obesity by educational campaigns will in practice increase the social divide and not help the poorer and more disadvantaged sectors of the population. It is therefore clear that in the modern world we need to recreate an environment where there is the opportunity to take physical activity routinely as part of daily living, not as an extra conscious decision which has to be made when there are so man other conflicting pressures.
The magnitude of the change in activity patterns can be seen in the steady collapse in physical activity with time and the almost routine fall in physical activity as people age. Some years ago we calculated that in the US there had been a fall amounting to 1,200 kcals per day in the energy used by men as they passed from a very active sporty life when they were 25 years old to the time when they were retired at 75 years of age (James et al., 1989). During this time mechanisation was in full swing so the secular decline of the whole population's activity was being amplified by the age related decline in spontaneous or sports related exercise. What this therefore means is that there will be an inevitable weight gain unless the same individuals - and indeed the total population systematically reduces their intake by many hundreds of kcals per day with a total drop for the elderly amounting to 1,200 kcals per day! It is not surprising therefore that as men and women give up sports in their early 20s then they gain weight progressively.
Urban design
Some cities, e.g. Copenhagen, Aarhus, Barcelona and many cities in the Netherlands are being maintained or redesigned to provide streets that are safe for children to play routinely outside the home, with special cycle paths and walkways for children to walk or cycle to school and where the elderly feel safe when they walk or cycle short distances to do their shopping. The design of cities with out-of-town supermarkets was an excellent idea for the interests of the supermarkets, but the public benefit was mainly felt by those with cars and the financial ability to shop once a week and store their food in large refrigerators. The poor with no transport and a family to feed found the small local shops disappearing or providing limited sources of food at higher prices. We need therefore to recognise that the decisions of local authorities on the development of congenial town centres with measures to facilitate local shops and with city centres for pedestrian and cycling only can be substantial contributors to an environment where physical activity is a routine rather than a special leisure time issue.
Work place policies to facilitate cycling and walking to work rather than car use
The French government and French local authorities as well as the business community could encourage physical activity by providing facilities at work which make it easier for people to cycle to work, store their bicycles, if need be take showers, and also possibly engage in physical activity at lunch time or after work. If one calculates the number of people employed by the public sector, then it is clear that the public sector could take a lead in changing the whole culture relating to physical activity. The business community could also be engaged if studies were undertaken to demonstrate to them the economic benefits that would arise if their employees were more active. Thus it is clear from a number of studies that both men and women feel better if they have been physically active and they then find it easier to work. Furthermore, there is now very substantial evidence to suggest that one can make a major difference in limiting the effects of high blood pressure, the development of diabetes and indeed of some cancers if people are more active. There are also a few studies which suggest that by encouraging physical activity the absenteeism and need for leave from work for hospital appointments etc. can be reduced. Given the fact that the major burden on European societies from obesity comes before retirement age and that physical activity is now clearly demonstrated to be of benefit, we need to take a very different strategic approach to providing the facilities and environment which positively encourages physical activity and limits routine car use.
The issue of schools will be dealt with separately.
The dietary challenge in France and the rest of Europe
There have been a number of major studies conducted by French investigators showing the value of a Mediterranean diet. New studies on the elderly reinforce the benefits of the Mediterranean diet which was characterised by substantial fruit and vegetable intake, i.e. a minimum of 400 g/day for every man, women and child. Traditionally the meat, milk, fat and sugar intake in the Mediterranean area was very low. Only in Greece was there a higher olive oil consumption and this population was heavier than the rest of the Mediterranean community when originally studied by Ancel Keys and his colleagues in the 1950s (Keys, 1980). The French culture, with its emphasis on the quality of food and the importance of regular family meals has probably made a major contribution to why the burden of disease in France and the obesity rates of the French have been lower than in many other European countries. Now, however, as described elsewhere by Inserm there is alarming evidence of an increase in overweight and obesity rates and this is now particularly affecting children. It would appear, therefore, that the French cultural tradition is being systematically destroyed by those forces that benefit when they successfully market new foods and soft drinks which are rich in fat and sugar and are therefore very dense in energy. This energy density, particularly when snacks and drinks are eaten between meals makes it extremely difficult for the normal brain mechanisms to control the body weight by shutting down food intake (Drewnowski, 1998; Stubbs et al., 1998; Raben et al., 2002; Prentice and Jebb, 2003). We therefore have in France at present a population where the normal brain mechanisms are telling the French to eat less because they are so physically inactive whilst at the same time the supermarket, retailing and other food sector strategies are encouraging the consumption of very inappropriate foods and drinks which do not conform with the quality of the traditional French cuisine. Again, therefore, as with the problem of physical inactivity, the idea of simply telling people to return to the marvels of traditional French cuisine naively neglects the huge pressures on society to "modernise" the French diet, this in practice meaning an encouragement to eat a far more obesity generating diet. The brain has particular difficulty in detecting fat in the diet and free sugars, especially if fats and sugars are taken between meals.
The price and availability of foods determines their consumption: implications of the Common Agriculture Policy
The evidence from behavioural studies on smoking, alcohol use and eating patterns all show that there are two fundamental factors which strongly influence the behaviour of a population, i.e. the price of a commodity (French et al., 2001) and the availability and marketing of these products. We must remember that the enormous benefits of the Common Agricultural Policy came when the needs of the poor farming community were matched with our original nutritional and health perceptions that children benefited from an ample supply of animal protein, e.g. in meat and milk, with sufficient energy being provided to ensure that even the poor could have enough to eat. The Post-War "cheap food policy" was introduced globally and the French government, as well as the other countries of the European community, have systematically subsidised the farming and food business in an effort to improve not only national food security but the well-being of the poorest in the community as well as the farming sector. As a result of many decades of huge subsidies for research and development and direct subsidies to encourage the production of meat, milk, cereal production (for animal feeding), oil and sugar production, France and the rest of the European community has an agricultural policy which is no longer geared to public health. Thus our agricultural colleagues recognised many years ago that farmers in the Mediterranean area would benefit from an increase in the price of fruit and vegetables and so they systematically funded from Brussels the destruction of most of the fruit and vegetables crops being grown in the Mediterranean (Robertson et al., 2004). This led to an increase in price which benefited the farmers but the higher price is a well-documented critical factor in limiting the choice of fruit and vegetables, particularly by the poor.
This example is simply used to show that industrial policies have a huge effect on health whether we are discussing transport and urban planning policies in relation to physical activity or agriculture and food policies in relation to the nutritional quality of the diet.
Post-war food industrial strategies
One of the major features of the post-war era is the huge development of the food and soft drink industries in North America and Europe. They have developed brilliantly by using a series of strategies to promote their sales:
• lower prices;
• ensuring that as many as possible outlets are available to the public;
• developing brands to promote their marketing;
• super sizing;
• focussing on preschool children marketing to induce brand loyalty and;
• selling their products in countries where they have low sales.
Originally food companies competed with each other by targeting the price of their commodity and to this day supermarkets highlight the price advantage of people buying from their particular supermarket chain. The food industry then realised that they could gain extra marketing advantage by ensuring that their products were available anywhere. Thus McDonalds in the US developed a strategy where everybody should be within a 5 min drive of a McDonald's restaurant and the same strategy is evident for all the major food companies. Then the marketers recognised the value of developing special brands of food; the marketing of brands has become a major preoccupation of most western industries. Following this there was the idea that one could market more effectively by "super-sizing", i.e. providing 50 % more or even twice as much for only a small increase in price. It is now well-documented that the bigger the portion of food presented to children over the age of 4 and to adults, the more they will spontaneously eat. When super-sizing was having no more impact, food companies and their advertising agents marketed the brands to children because they discovered that children could have a profound influence on their parents' purchases and supermarkets learned the tricks needed to persuade their parents to buy particular food, confectionery and soft drinks.
Now the next industrial strategy for most big food companies is to target those areas of the Mediterranean and developing countries where their products are not yet being consumed. This has therefore led to a dramatic reduction in the quality of the Mediterranean diet with a marked increase in fat and sugar intakes. This has particularly affected children so that in many Mediterranean countries the children now have hamburgers, fried foods, soft drinks, sweets, chocolate and biscuits. They are being targeted with the idea that snacks and soft drinks and fast foods are an appropriate part of an enjoyable life and new evidence is emerging that children no longer are being brought up in the traditional environment where they would be exposed as a routine to set meals rich in fruit and vegetables with very few high fat foods and practically no added sugar. It is now well recognised that children need to be exposed to vegetables and fruits for up to 15 times before they accept these foods as a normal part of their diet. Fats, sugars and salt, however, are tastes for which we have primitive drives with special taste buds and mouth sensing systems geared in evolutionary terms to targeting these sources of energy and salt needs. Now, however, these primitive drives are being used to market products because taste panels routinely show the attractiveness of products rich in these ingredients.
Developing prevention strategies relating to the quality of food
Figure 2 shows a general scheme for providing a coherent approach to changing the environment both in terms of physical activity and diet. The emphasis so far has been primarily confined to the idea that an educational approach is all that is necessary, but the latest rigorous Cochrane analysis shows that advice to individuals, even given by doctors has, as a population approach, very little effect (Brunner et al., in press). Thus we have to now focus on changing the environment at a physical, economic, political, i.e. legislative and regulatory level, as well as considering how best to change the accepted cultural perceptions of fast foods, snacking, soft drink consumption and eating on the move, all of which are conducive to weight gain. Table 1 provides an indication of how food pricing and availability policies could be developed progressively over a 5-10 years period. Indeed the French parliament, with its traditional concern for both the quality of French food, its cultural associations and the well-being of farmers could make a major contribution to spearheading a new approach to obesity prevention in the European Community.
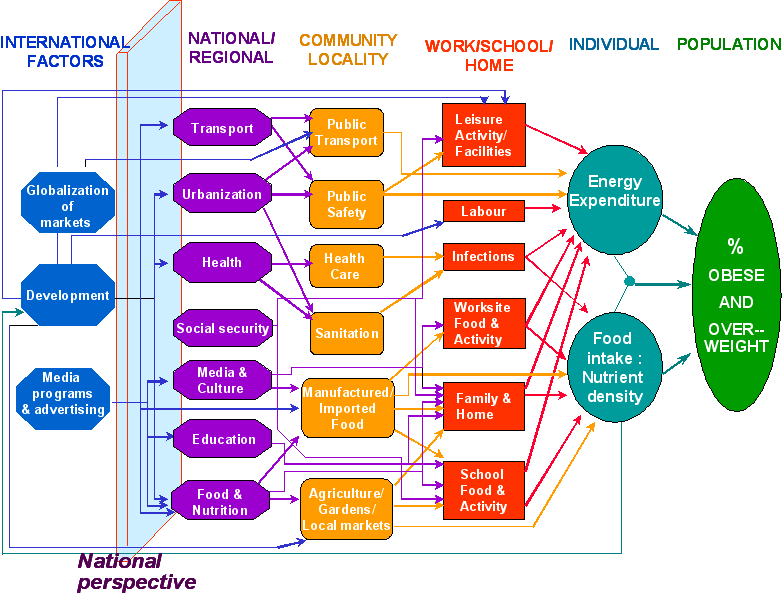
Figure 2 : Societal policies and processes influencing the population prevalence of obesity
This figure illustrates the numerous factors and sites which in practice influence the choice of activity and foods by individuals. Therefore no one solution to the problem of excess eating and physical inactivity can be expected (Kumanyika et al., 2002).
Modified from Ritenbaugh C, Kumanyika S, Morabia A, Jeffery R, Antipatis V. IOTF website 1999: http://www.iotf.org
Table 1 : Food "availability" and pricing policies
|
Clear evidence of need for training young children to eat fruit and vegetables: 10-15 exposures to food needed before acceptance assured. Food environment crucial |
|
Implies major controls on marketing - not just advertising - to children. Overwhelming evidence that regulatory rather than voluntary controls needed to benefit respectable food companies |
|
Weaning practices and pre-school food - not just nutrition standards now required to control total food availability to children as part of ensuring an appropriate environment |
|
Total control of school premises and their surroundings now needed with a transformation of food practices in school - Chef Jamie Oliver in UK highlights value of no processed foods and involving children in origin etc. of food and enhancing the power, training and prestige of food organisers. The curriculum on food also needs. Transforming in the UK |
|
All Government controlled or influenced food systems, e.g. hospital premises, should control junk food and soft drink availability, as for alcohol and tobacco |
|
Criteria needed for quality of food served in all work place initiatives |
|
Major new initiative to define "Junk foods" and limit their availability in all town centres - i.e. like alcohol outlets and smoking: can use pricing policies as a mechanism also. Include environmental concerns - limit take away foods to reduce litter... |
|
Limit fast foods and drink availability in town centres through planning policies or if need be by taxing the licence for premises as a new policy |
|
Fat and sugar taxes need to be assessed by economists using classic evidence on price flexibility |
|
Need nutritional profiling in food labels relating to energy density with additional nutritional criteria as a technique for setting new standards for food - targeting "junk foods" and energy rich drinks |
|
Finnish development of incorporating the price of a salad bar and the choice of vegetables within the cost of the main meal dramatically increased national fruit and vegetable consumption 3 fold |
|
Nordic country agriculture initiatives were used to lower prices of fruit and vegetable prices in more remote areas |
|
Reconsider legacy of EU distortion of food prices: now promote local vegetable and fruit production and distribution/storage systems to facilitate cost effective help for Northern and poor communities |
|
Regear tax policies on foods: needs novel political educative initiatives |
|
Consider import taxes and role of phytosanitary regulations in World Trade Organisation rules on free trade to ban or heavily tax health threatening imports of inappropriate foods. Appeals by US and others invoking reference to CODEX system will thereby require WHO and FAO to validate health issues - already specified in WHO 916 report |
Food labelling
Food labelling is but one example where the idea that the public is able to discriminate the quality of food on the basis of the current labelling system has proven to be wrong. Repeated consumer surveys show that consumers cannot understand the labels which are set out in technical jargon and the idea of specifying what an average man or women needs in terms of energy is not only wrong and misleading, but ludicrous! The energy needs of children and adults can vary threefold and if the public, with great difficulty, managed to follow the advice implied by the need of women for 2,000 kcals and men for 2,500 kcals, then if these were the average need of French men and women, which I doubt, then by following the advice meticulously almost half the French population would start gaining weight, and almost half losing weight. This is why the British Parliamentary Health Committee on the basis of extensive consumer research and analyses by the Food Standards Agency of the UK (Rayner et al., 2004), advocated the use of a traffic light type of signalling system whereby consumers could distinguish the overall quality of the food itself based on scientific analyses of the food's quality in terms of fat, sugar and salt. A red signalled food should be eaten sparingly, green labelled foods in abundance and yellow labelled foods in moderation. Currently the European Commission is considering the need to have some simple method which highlights the nutritional and health quality of a food but all too often food companies are only interested in marketing their good foods as "functional foods" of value, whilst ignoring the fact that many of their products should be eaten sparingly, if at all. The nutritional profile of foods is important and it is no longer possible for industrial interests to argue that there are no good foods or bad foods; by definition if one food is considered better than another for its nutritional and health properties, then it should be possible to a develop a uniform and systematic labelling of foods, and certainly of particular dishes in canteens, the workplace, restaurants as well as in supermarkets.
Table 2 shows a proposed list of strategies for helping to prevent obesity in children and a list of policies in schools which have been proposed and/or tried successfully. There is ample evidence that children below the age of about 12 have not yet developed the ability to make an appropriate judgement where they can discriminate between a marketing message geared to their immediate desires and a more rational long-term and coherent view of the different opinions that one will encounter in everyday life. Thus experts in child psychology and paediatrics have emphasised the importance of creating an environment which is appropriate for a child's learning. Currently it seems to have been accepted that the unbridled marketing of products to children is acceptable when this in practice is manipulating children's behaviour for the benefit of the marketeer without regard to the long-term welfare of the child. This is not a controversial judgement but was clearly set out in a special report which took account of the world's literature on the ability of children to understand the information that they receive on food. It became clear after consulting about 30,000 published references that the marketing of a brand not only enhances the demands of children for that selected item, but it also increases their desire for the category of products, e.g. soft drinks, which are being marketed. This in turn leads to a change in the categories of food consumed and a distortion of the nutritional quality of a young child's diet. It has been recognised for a long time that children brought up in a very organised and socially-advantaged environment are able to maintain their activity and food patterns much more effectively, despite external pressures to change, providing that they are protected from inappropriate influences before they go to school and throughout the primary school period. Only when they are going through their adolescent development does the normal interplay of the home environment and external influences become and issue. Therefore it is clear that we have, in the last two to three decades, failed to understand the fundamental importance of protecting our children from the inappropriate marketing of foods which are disadvantageous to their health. Overweight children already show the accelerated responses indicative of the early phases in the development of diabetes and high blood pressure. Thus the progressive increase in the rates of overweight and obesity in France should be of major concern. It is obviously completely inappropriate to blame the child and the idea that parents have complete control over the well-being of their children is no longer true when so many families have both parents at work. Table 2 summarises the variety of initiatives which can be undertaken to change children's environment.
Table 2 : Strategies for combating childhood obesity
|
Protecting children aged up to 12 years |
School environment |
|
New evidence from WHO of the fundamental need for 6 months' breast feeding implies transformation of individual paediatric advice to mothers about overweight |
No "choice" in food menus so that young children are trained in appropriate food selection! |
|
Proper weaning practices |
No vending machines |
|
Overwhelming evidence of need to exclude children from "choice" option when young, e.g. <8 years (American Paediatric and Psychological Societies) or before 12 -14 years based on understanding of the biological development and mental processing capacity of children (Hastings et al., 2003, UK). |
Activities and sports for all: not just the very athletic - ensure the opportunity for after school activities |
|
Regulated child minders: food and play |
Defined high quality meals only should be served |
|
Legislate on all forms of marketing: TV, radio, text messages, internet, food product labelling, games etc. |
Contracts with parents on food are needed in supporting high quality foods in school with no additional confectionary etc allowed on school premises |
|
School environment needs changing to prevent any inappropriate exposure |
Food and activity committee with Governor, pupil and parent representation shown to transform school practices |
|
Supermarket practices need to stop manipulating children to buy inappropriate foods |
Nutrition education needs transforming with explicit messages and practical experience of foods such as fruits, vegetables, cooking techniques and the origins and biological effects of foods |
|
Pricing policies: affect school aged children |
Parental educational initiatives by children needed routinely as in Finnish salt experience |
|
Availability policies: density of fast food outlets needs to be limited where children frequently go |
School teachers eating with children plays major role in modelling behaviour |
|
Walk/bike to school: needs to be encouraged with suitable changing and bike and clothes storage facilities |
|
|
Traffic policies around school need explicit consideration |
|
|
Parental policies on transport to school needs to be considered - parents protect their children by driving them to school thereby making it more dangerous for other children! |
Conclusions
It is no longer possible to argue that an educational approach to individual behaviour is the answer to the obesity epidemic. French children need to be protected and the biggest drive in educational terms should be not simply to the school children but to policy makers in the areas of fiscal, agriculture, retailing, transport, urban design and education policies. Table 3 simply summarises the fact that one should not only think of the Ministry of Health as responsible for the obesity epidemic: the other Ministries of Government have a far greater influence on the development of the obesity epidemic than the Health Ministry. The Ministry of Health is now trying to cope with the immensely deleterious effects of other government departments' policies over several decades. The French nation, like other western countries, will not be able to afford the escalating health costs. Without a new strategy approach with multiple interventions in many different sectors, it is unlikely that we can stem the obesity epidemic. There is no single magic bullet and a coherent plan is now needed with a careful monitoring and evaluation of the different initiatives. Other governments, e.g. Sweden, have just produced their new plan of action and France has an opportunity once again to lead the European Community in developing new strategies of benefit to even the poorest in society.
Table 3 : The Stefani model: a few examples of strategies for effective nutritional initiatives to illustrate the different dimensions of policy needed
|
Ministry of Health Responsibilities |
Other Ministry responsibilities |
|
|
Physical |
Dietary quality; physical activity |
Dietary quality; physical activity |
|
Appropriately accessible health centres Promoting access to appropriate self-monitoring, e.g. weight, BP |
Ensuring playgrounds in schools, suitable cycling and road systems; urban planning; sports facilities. Designated urban areas for local food production |
|
|
Economic |
Primary health payments for specific targets in management |
Re-evaluate taxation and subsidy policies |
|
Policy |
Baby Friendly Hospitals Dietary guidelines establishing fortification policies Establish policies on health claims, e.g. functional foods |
HIA of CAP Food labelling with appropriate, understandable health related information |
|
Socio-cultural |
Health education |
Promote physical activity in the workplace. Create breastfeeding time and space in the workplace with NGO help |
W. Philip T James
Chairman,
International Obesity Task Force
and the London School of Hygiene and
Tropical Medicine
REFERENCES
BRUNNER E et al. Cochrane analysis of the impact of individual dietary advice on health changes. In press .
DEPARTMENT OF HEALTH. Choosing health. Making healthy choices easier. White Paper on Public Health. HMSO, Norwich, UK, 2004 www.tso.co.uk/bookshop
DREWNOWSKI A. Energy density palatability and satiety: implications for weight control. Nutrition Reviews 1998, 56 : 347-353
EURODIET. Reports and Proceedings. Also Volume 4(2B) April 2001: Nutrition and Diet for Healthy Lifestyles in Europe: the EURODIET evidence. Public Health Nutrition. 4 (2A) April 2001
FOOD AND AGRICULTURAL ORGANIZATION OF THE UNITED NATIONS. Human Energy Requirements. FAO. Food and Nutrition Technical Report Series 1 Report of a Joint FAO/WHO/UNU Expert Consultation. Rome, 17-24 October 2001
FRENCH SA, JEFFERY RW, STORY M, BREITLOW KK, BAXTER JS, HANNAN P, SNYDER MP. Pricing and promotion effects on low-fat vending snack purchases: the CHIPS Study. Am J Public Health 2001, 91 : 112-117
HASTINGS G, STEAD M, MCDERMOTT L, FORSYTH A, MACKINTOSH AM, et coll. Review of research on the effects of food promotion to children. Final report prepared for the Food Standards Agency, 2003 http://www.food.gov.uk/multimedia/pdfs/foodpromotiontochildren1.pdf
HOUSE OF COMMONS HEALTH COMMITTEE. Obesity: Third Report of Session 2003-04, Volume I. Report, together with formal minutes. The House of Commons. HC 23-I. Published on 27 May 2004, The Stationery Office Limited, London
JAMES WPT, RALPH A, FERRO-LUZZI A. Energy Needs of the Elderly: A new approach. In Nutrition, Aging, and the Elderly. MUNRO HN, DANFORD DE (eds). Plenum Press, New York and London, 1989 : 129-151
JAMES WPT, MCCOLL K. A Food Standards Agency for the UK. A report for the Prime Minister. HMSO London, 1997
JAMES WPT, JACKSON-LEACH R, NI MHURCHU C, KALAMARA E, SHAYEGHI M, et coll. Overweight and obesity (high body mass index). In : Comparative Quantification of Health Risks. Global and Regional Burden of Disease Attributable to Selected Major Risk Factors. EZZATI M, LOPEZ AD, RODGERS A, MURRAY CJL (eds). Chapter 8, Volume 1. World Health Organization, Geneva, 2004
KEYS A. Seven countries. A multivariate analysis of death and coronary heart disease. Cambridge, MA, US, Harvard University Press, 1980
KUMANYIKA S, JEFFERY RW, MORABIA A, RITENBAUGH C, ANTIPATIS VJ. Public Health Approaches to the Prevention of Obesity (PHAPO) Working Group of the International Obesity Task Force (IOTF). Obesity prevention: the case for action. Int J Obes Relat Metab Disord 2002, 26 : 425-436
NATIONAL AUDIT OFFICE. Tackling obesity in England. A report by the Comptroller and Auditor General. National Audit Office, London, 2001
PRENTICE AM, JEBB SA. Fast foods, energy density and obesity: a possible mechanistic link. Obes Rev 2003, 4 : 187-194
RABEN A, VASILARAS TH, MOLLER AC, ASTRUP A. Sucrose compared with artificial sweeteners: different effects on ad libitum food intake and body weight after 10 wk of supplementation in overweight subjects. Am J Clin Nutr 2002, 76 : 721-729
RAYNER M, SCARBOROUGH P, STOCKLEY L. Nutrient profiles: options for definitions for use in relation to food promotion and children's diets. FSA, London, 2004
ROBERTSON A, TIRADO C, LOBSTEIN T, JERMINI M, KNAI C, et coll. Food and Health in Europe: A new basis for action. WHO Regional Publications. European Series, 96, Copenhagen, 2004
STUBBS RJ, JOHNSTONE AM, O'REILLY LM, BARTON K, REID C. The effect of covertly manipulating the energy density of mixed diets on ad libitum food intake in `pseudo free-living' humans. International Journal Obesity & Related Metabolic Disorders 1998, 22 : 980-987
WANLESS D. Securing Good Health for the Whole Population. Final Report, February 2004. www.hm-treasury.gov.uk.
WHO. Diet, Nutrition and the Prevention of Chronic Diseases. WHO Technical Report, Series 797. World Health Organization, Geneva, WHO, 1990
WHO. Obesity: preventing and managing the global epidemic. WHO Technical Report Series N o 894, WHO, Geneva, November, 2000
WHO. Diet, Nutrition and the Prevention of Chronic Diseases. Report of a Joint WHO/FAO Expert Consultation. WHO Technical Report Series No. 916. World Health Organization, Geneva, 2003